Osteoarthritis, often referred to as OA, is a degenerative joint disease that primarily affects the cartilage, the protective tissue that covers the ends of bones in a joint. It is the most common type of arthritis and is typically associated with aging, although it can also occur due to joint injury, obesity, or genetic factors. Here’s some more information about osteoarthritis.
Osteoarthritis – Everything You Need To Know

Causes of Osteoarthritis
- Age: The risk of developing osteoarthritis increases with age, as the cartilage naturally deteriorates over time.
- Joint injury: Trauma to a joint, such as a fracture or ligament tear, can increase the likelihood of developing osteoarthritis.
- Obesity: Excess weight places additional stress on your joints, particularly the knees and hips, resulting in a higher risk of developing osteoarthritis.
- Genetics: Certain genetic traits can make individuals more susceptible to osteoarthritis.
Related: Tendonitis – Everything You Need to Know
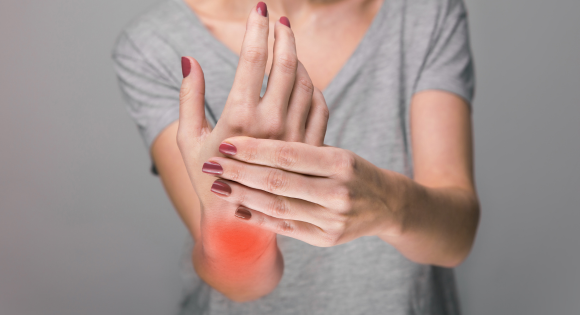
Symptoms of Osteoarthritis
- Joint pain: The most common symptom of osteoarthritis is pain in the affected joint. The pain is typically described as a deep ache that worsens with activity.
- Stiffness: Affected joints may feel stiff, especially in the morning or after periods of inactivity. The stiffness usually improves with movement.
- Limited range of motion: Osteoarthritis can cause a reduced range of motion in the affected joint, making it difficult to fully bend, straighten, or rotate it.
- Swelling: Inflammation may occur in the joint, leading to mild swelling and tenderness.
Diagnosis of Osteoarthritis
Diagnosing osteoarthritis typically involves a combination of medical history, physical examination, and imaging tests. X-rays can reveal joint damage, such as narrowing of the joint space, bone spurs, or the presence of extra fluid. Sometimes, other imaging tests like magnetic resonance imaging (MRI) or ultrasound may be used for a more detailed evaluation.
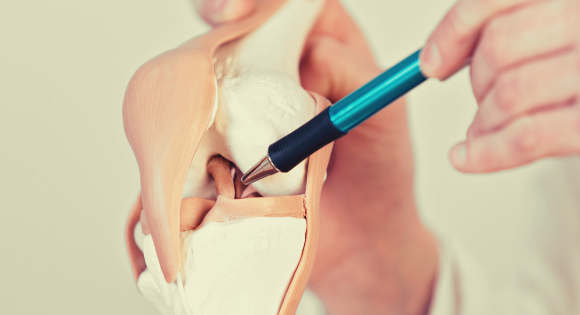
Complications
Osteoarthritis can lead to certain complications over time, including:
- Reduced quality of life: Chronic pain and limited mobility can impact a person’s overall quality of life, making it difficult to perform daily activities or participate in recreational or social pursuits.
- Disability: In severe cases, osteoarthritis can cause significant joint damage, leading to joint deformity and functional disability. This can affect a person’s ability to work or carry out independent tasks.
- Joint instability: As osteoarthritis progresses, the stability of the affected joint may be compromised, increasing the risk of falls or further injury.
- Emotional impact: Living with chronic pain and physical limitations can have emotional consequences, such as depression, anxiety, or frustration.
Prevention
While osteoarthritis cannot always be prevented, certain measures may help reduce the risk or delay its onset:
- Maintain a healthy weight: Excess weight adds pressure on the joints, particularly the weight-bearing joints like the knees and hips. If necessary, maintaining a healthy weight or losing weight can help reduce the strain on the joints.
- Exercise regularly: Regular physical activity, such as low-impact exercises or strength training, can help strengthen the muscles around the joints and improve joint stability.
- Protect your joints: When engaging in activities that may stress the joints, such as sports or manual labor, use appropriate protective equipment and techniques to minimize the risk of injury.
- Avoid repetitive joint stress: Prolonged and repetitive stress on a joint can contribute to osteoarthritis. If your occupation or hobbies involve repetitive motions, take regular breaks or modify your technique to reduce joint strain.
- Good posture: Maintaining good posture and body mechanics can help distribute weight and stress evenly across the joints, reducing the risk of excessive wear and tear.

Treatment
- Medications: Over-the-counter pain relievers (e.g., acetaminophen, nonsteroidal anti-inflammatory drugs) can help manage pain and inflammation. Sometimes, prescription medications, such as stronger pain relievers or corticosteroids, may be necessary.
- Physical therapy: Exercises and physical therapy can improve joint strength, flexibility, and function.
- Lifestyle modifications: Maintaining a healthy weight, engaging in low-impact exercises (e.g., swimming, cycling), and using assistive devices (e.g., braces, canes) can reduce joint stress.
- Injections: Corticosteroid injections or hyaluronic acid injections may be used to provide temporary pain relief.
- Surgery: In severe cases where conservative measures are insufficient, surgical interventions like joint replacement may be considered.
Final Thoughts
It’s important to note that while osteoarthritis cannot be cured, its symptoms can be managed effectively with appropriate treatment and lifestyle modifications. Consulting with a healthcare professional is recommended for an accurate diagnosis and personalized treatment plan.
Sending you plenty of light, love, and healing-inducing vibes!
Anthea

